Using Device Registries to Generate Clinical Evidence for EU MDR Certification
Article Summary
EU MDR 2017/745 significantly elevates the role of medical device registries as sources of real-world clinical evidence across the product lifecycle. While registries offer powerful advantages for post-market surveillance and continuous compliance, their regulatory value depends on data quality, governance, and alignment with standards such as ISO 14155.Article Contents
Introduction
The European Union Medical Device Regulation, EU MDR 2017/745 (European Commission, 2017), includes a significantly strengthened framework for medical device safety and performance evaluation, and post-market surveillance (PMS). Registries as structured systems for collecting real-world clinical data are increasingly recognised as high value sources of clinical evidence that can be utilised for the conformity assessment process. The MDR explicitly encourages the establishment of device registries and databanks to support vigilance, traceability, post-market clinical follow-up (PMCF), and ongoing benefit-risk evaluation (Article 108). Annex VII also outlines that Notified Bodies should consider registry data submitted by the manufacturer for the renewal of MDR certificates.
Although registries existed long before the MDR, their use is often fragmented, inconsistent, or limited to specific clinical communities (e.g. joint replacement implants). Under the MDR, they now carry far greater regulatory relevance because manufacturers must provide continuous clinical evidence throughout the device lifetime, including real-world safety and performance data. For many devices, especially implants, well-established technologies, orphan devices, and products with limited premarket evidence, registry data can be used to demonstrate compliance with the General Safety and Performance Requirements (Annex I – GSPRs).
MDR Requirements for Clinical Evidence and PMS
The MDR requires a structured, transparent and robust clinical evaluation process, ideally including real-world data sources. Article 61 requires that manufacturers demonstrate conformity with the GSPRs using sufficient clinical evidence proportional to the risk classification and novelty of the device. Registry data are explicitly recognised as valid clinical evidence sources.
If available, manufacturers must integrate registry data into:
- Clinical Evaluation Reports – CERs (European Commission, 2016)
- Post-Market Clinical Follow-Up (PMCF) activities, Annex XIV (Medical Device Coordination Group, 2020a, 2020b, 2020c)
- Periodic Safety Update Reports (PSURs) for Class IIa, IIb, and III devices (Medical Device Coordination Group, 2022)
- Summary of safety and clinical performance – SSCP (Medical Device Coordination Group, 2019)
- Post market surveillance (PMS), safety signal detection and trend analysis (Medical Device Coordination Group, 2025 and Badnjević, 2022)
- Risk management updates (International Organisation for Standardisation, 2019)
- ISO 13485 quality management system (QMS) processes including Design Validation and Feedback – clauses 7.3.7 and 8.2.1 respectively (International Organisation for Standardisation, 2016)
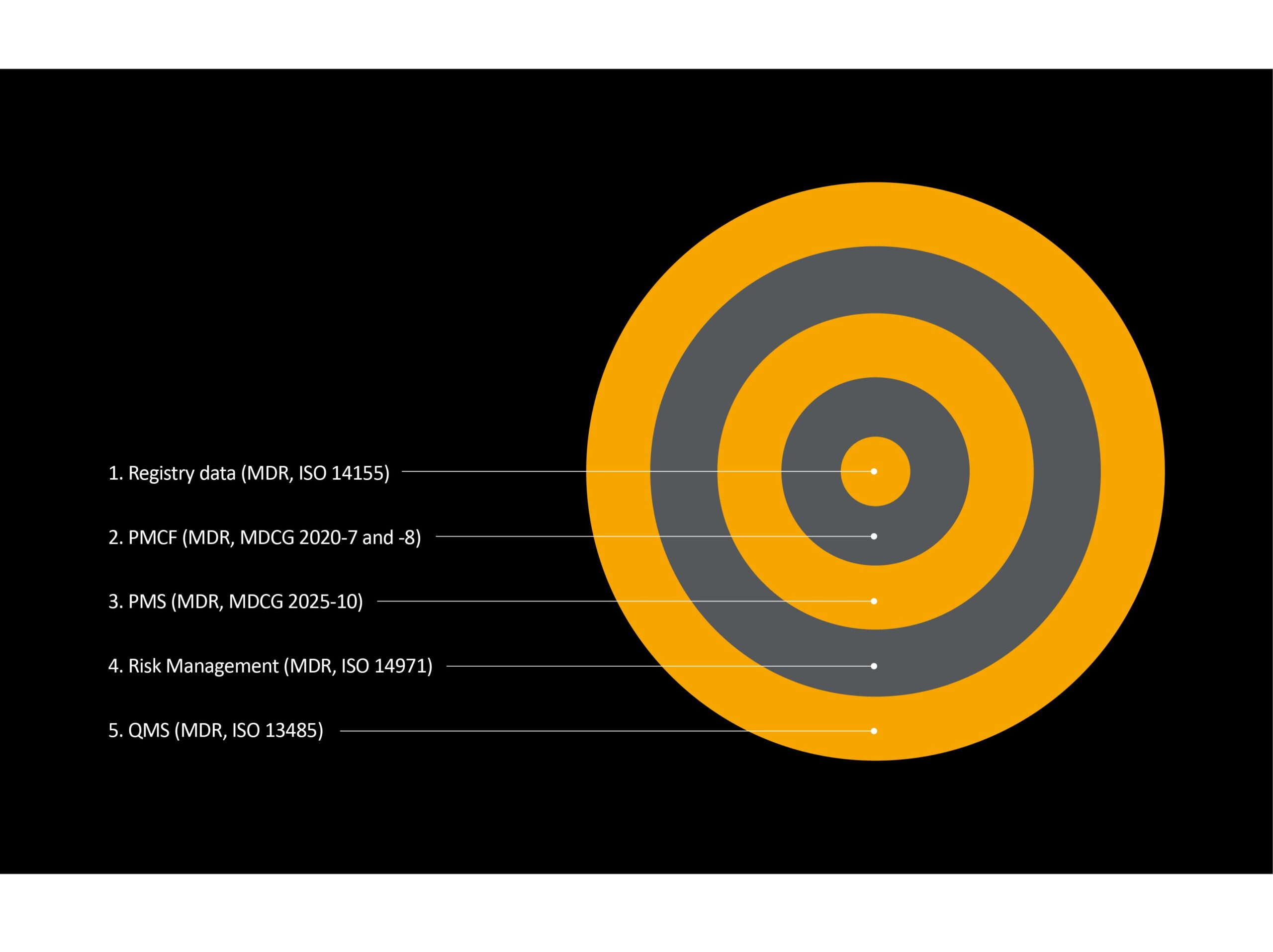
Figure 1 – Hierarchy showing relationship between registry data to other process in the manufacturers QMS. Output and updates to these processes feed into documentation updates over the device lifetime such as CER, SSCP and PSUR.
Registries can be considered a high-quality clinical data (Rank 3 from Appendix III of MDCG 2020-09 in terms of level of evidence) collection system in the post-market phase to support clinical benefits (Medical Device Coordination Group, 2020c) with real-world data for MDR submissions to Notified Bodies and other global regulators (Food and Drug Administration, 2025 and Dang, 2023). Registries can support these obligations by providing large-scale, longitudinal, real–world datasets, which may be impossible to acquire through conventional clinical studies alone (Sedrakyan, 2022, Beit Ner, 2022, Rubinger, 2023 and Doherty, 2023).
ISO 14155 and Its Relevance to Registries
ISO 14155:2020 (International Organisation for Standardisation, 2020) provides the international standard for Good Clinical Practice (GCP) in medical device clinical investigations. While the standard mainly governs interventional clinical investigations, many of its principles apply directly to registry-based research, registry-embedded RCTs (Doherty, 2023), or PMCF activities conducted within registries. Registries are also outlined in Annex I of ISO 14155 as an integral part of the post-market clinical development stage.
According to ISO 14155, clinical studies must:
- Protect the rights, safety, and wellbeing of human subjects
- Ensure scientific validity and credibility of results
- Clearly define responsibilities of sponsors, investigators, and monitors
- Establish proper protocols, data quality systems, and monitoring
Registries that aim to support MDR certification should therefore reflect ISO 14155 principles where applicable, especially regarding data integrity, ethics approvals, informed consent, monitoring procedures, endpoint definitions, and documentation.
Types and Functions of Device Registries
The literature identifies multiple registry types: disease-based, procedure-based, pathology-specific, product-focused, or hybrid ecosystems linking multiple datasets. Examples include joint arthroplasty (Beit Ner, 2022 and Hallstrom, 2022), cardiovascular (Batra, 2023, Hoogervorst, 2023 and Malenka, 2022), spine (Quigley, 2023 and Pascucci, 2023), neurology (Lee, 2021) and dental implant (Berge, 2025 and Naemi, 2021) registries. These device-specific registries will be explored in greater detail in Part 2 of this article series.
Registries serve several regulatory-relevant functions:
- Collecting real-world performance data (Dang, 2023)
- Monitoring adverse events and revisions (Hoogervorst, 2023)
- Identifying early device failures (Beit Ner, 2022)
- Benchmarking implants, techniques, centres, and operators (Hallstrom, 2022)
- Supporting RWE-based decision-making at system and regulatory levels (Dang, 2023)
The MDR’s emphasis on continuous lifetime evidence makes these functions indispensable as a clinical data source for MDR certification.

Strengths of Using Registry Data for MDR Evidence
Registries have several advantages over traditional clinical studies:
- Large, diverse populations enabling generalizable conclusions (Rubinger, 2023) often exceeding patient numbers in clinical investigations and post-market studies
- Long-term follow-up extending far beyond typical premarket trials (Rubinger, 2023)
- Cost efficiency (Giori, 2021), also illustrated by registry-based RCTs (e.g., TASTE trial – Rubinger, 2023)
- Detection of rare events (Doherty, 2023) and device failures (Beit Ner, 2022), e.g. metal-on-metal hips, ASR recall
- Integration with EHRs (Giori, 2021), PROMs (Boyle, 2021), and UDI systems
- High external validity, reflecting real-world clinical practice (Dang, 2023)
- Comparisons between countries / markets
- Collection and stratification of data on device variants / sub-variants
These characteristics align well with MDR expectations for collecting clinical data, PMCF and ongoing risk-benefit evaluation.
Limitations and Challenges
Despite their value, registries also face challenges that must be considered if the data is used to support MDR certification:
- Heterogeneity in data collection (Quigley, 2023), variables, outcomes, and definitions across Europe (Rubinger, 2023)
- Incomplete coverage (Rubinger, 2023) and data quality gaps, particularly in cardiovascular registries (Hoogervorst, 2023)
- Passive follow-up underestimates adverse events (Rubinger, 2023) and a lag between safety events and identification and actions by the registry
- Lack of standardised outlier definitions across registries (Hoogervorst, 2023)
- Variable enforcement of data entry (Rubinger, 2023)
- Potential selection, reporting, and measurement biases (Dang, 2023 and Doherty, 2023)
- Funding dependence and the risk of conflicts of interest in industry-supported registries (MedTech Europe, 2017)
- Small number effects which can lead to aspects such as false positives and / or low statistical power
These limitations may affect the reliability and regulatory acceptability of registry data and provide areas of focus for the strategic development of future registries (covered further in Part 3 of this article series).

Quality Requirements for MDR Use of Registry Data
For registry data to meaningfully support conformity assessment, manufacturers should evaluate the registry according to key criteria identified in the literature and regulatory guidance:
- Coverage – ideally ≥95% patient/procedure inclusion, per IMDRF (Hoogervorst, 2023)
- Data completeness – e.g. a variable will only be analysed if completeness is ≥95% (Hoogervorst, 2023)
- Accuracy and validation procedures – audits, monitoring, UDI traceability (European Commission, 2015)
- Consistency of definitions, outcomes, and timepoints (MedTech Europe, 2017)
- Robust governance and data protection mechanisms – GDPR (MedTech Europe, 2017)
- Links to other datasets – EHR, national registries, mortality data (Gliklich, 2014)
High-quality registries could increasingly serve as an essential component of MDR clinical evidence strategies.
Notified Body Experience of Registry Data
Within the Orthopaedic team at BSI, there is extensive experience in evaluating registry data to support MDR certification. This includes input from clinicians with previous direct involvement in the UK National Joint Registry (NJR). Based on our experience with the NJR and other international joint replacement registries, several recurring considerations commonly arise:
- PROMs data is often limited. While survival rates and reasons for revision are usually well captured as safety outcomes, there is frequently far less reporting of patientreported outcome measures (PROMs), which are key indicators of device performance.
- Data stratification requires careful balance. Differentiating between implant variants and indications is essential, but excessive granularity can reduce the statistical power and scientific robustness of the analysis.
- Predicting early sales and registry uptake is challenging. For new products undergoing initial MDR certification, manufacturers may struggle to anticipate market adoption in individual countries making it difficult to forecast how much registry data will be available in the early years.
- Manufacturers often see deeper insights than regulators. Many registry systems provide manufacturers with access portals containing more detailed, realtime data on their devices than what appears in public reports or is accessible to regulators, creating an important dynamic in evidence interpretation.
Conclusions
As the MDR continues to reshape the regulatory landscape for medical devices, registries have evolved from optional data collection resource into critical pillars of lifecycle evidence generation. Their ability to provide comprehensive, longitudinal, real‑world data makes them uniquely positioned to support continuous assessment of safety, performance, and clinical outcomes – core expectations within the MDR framework. While challenges remain, particularly regarding data quality, harmonisation, governance, and consistent methodology, well‑designed registries that align with recognised standards and principles are increasingly becoming essential tools for manufacturers seeking to demonstrate ongoing compliance with the GSPRs. By integrating registry evidence across CERs, PMCF, PMS, and broader risk‑management processes, manufacturers can not only meet regulatory obligations but also contribute to improved patient safety, better device transparency, and higher‑quality clinical care across Europe and other jurisdictions.
Read more about specific medical device examples in Part 2: Using Device Registries to Generate Clinical Evidence for EU MDR Certification: Specific Devices
Read more about the future of medical device registries in Part 3: Using Device Registries to Generate Clinical Evidence for EU MDR Certification: The Future of Registries
References
- Badnjević, A., Pokvić, L. G., Deumić, A., & Bećirović, L. S. (2022). Post-market surveillance of medical devices: A review. Technology and health care : official journal of the European Society for Engineering and Medicine, 30(6), 1315–1329. https://doi.org/10.3233/THC-220284
- Batra, G., Aktaa, S., Wallentin, L., Maggioni, A. P., Wilkinson, C., Casadei, B., & Gale, C. P. (2023). Methodology for the development of international clinical data standards for common cardiovascular conditions: European Unified Registries for Heart Care Evaluation and Randomised Trials (EuroHeart). European Heart Journal – Quality of Care and Clinical Outcomes, 9(2), 161-168. https://doi.org/10.1093/ehjqcco/qcab052
- Beit Ner, E., Nakamura, N., Lattermann, C., & McNicholas, M. J. (2022). Knee registries: State of the art. Journal of ISAKOS, 7(5), 118-131. https://doi.org/10.1136/jisakos-2021-000625
- Berge, T. L. L., Lygre, G. B., Kubon, B., & Lie, S. A. (2025). Key factors for a national dental implant registry. Journal of Dentistry, 154, 105603. https://doi.org/10.1016/j.jdent.2025.105603
- Boyle J. R. (2021). Future of surgical registries. The British journal of surgery, 108(7), 740–741. https://doi.org/10.1093/bjs/znab176
- Dang A. (2023). Real-World Evidence: A Primer. Pharmaceutical medicine, 37(1), 25–36. https://doi.org/10.1007/s40290-022-00456-6
- Doherty, D. A., Tong, S. Y. C., Reilly, J., Shrapnel, J., McDonald, S., Ahern, S., Harris, I., Tam, C. S., Brennan, A. L., Hodgson, C., Wilcox, L., Balagurunathan, A., Butcher, B. E., & Reid, C. M. (2023). Registry randomised trials: a methodological perspective. BMJ open, 13(3), e068057. https://doi.org/10.1136/bmjopen-2022-068057
- European Commission (2015) Methodological guidelines and recommendations for efficient and rational governance of patient registries https://health.ec.europa.eu/publications/methodological-guidelines-and-recommendations-efficient-and-rational-governance-patient-registries_en
- European Commission. (2016). Clinical evaluation: a guide for manufacturers and notified bodies under directives 93/42 and 90/385 (MEDDEV 2.7/1 revision 4) https://ec.europa.eu/docsroom/documents/17522/attachments/1/translations
- European Commission. (2017). Regulation (EU) 2017/745 of the European Parliament and of the Council of 5 April 2017 on medical devices (2017/745) https://eur-lex.europa.eu/eli/reg/2017/745/oj/eng
- Food and Drug Administration. (2025). Use of Real-World Evidence to Support Regulatory Decision-Making for Medical Devices – Guidance for Industry and Food and Drug Administration Staff https://www.fda.gov/media/190201/download
- Giori, N. J., Radin, J., Callahan, A., Fries, J. A., Halilaj, E., Ré, C., Delp, S. L., Shah, N. H., & Harris, A. H. S. (2021). Assessment of Extractability and Accuracy of Electronic Health Record Data for Joint Implant Registries. JAMA network open, 4(3), e211728. https://doi.org/10.1001/jamanetworkopen.2021.1728
- Gliklich, R. E., Dreyer, N. A., & Leavy, M. B. (Eds.). (2014). Registries for Evaluating Patient Outcomes: A User’s Guide. (3rd ed.). Agency for Healthcare Research and Quality (US).
- Hallstrom, B. R., Hughes, R. E., & Huddleston, J. I., 3rd (2022). State-Based and National U.S. Registries: The Michigan Arthroplasty Registry Collaborative Quality Initiative (MARCQI), California Joint Replacement Registry (CJRR), and American Joint Replacement Registry (AJRR). The Journal of bone and joint surgery. American volume, 104(Suppl 3), 18–22. https://doi.org/10.2106/JBJS.22.00564
- Hoogervorst, L. A., Geurkink, T. H., Lübbeke, A., Buccheri, S., Schoones, J. W., Torre, M., Laricchiuta, P., Piscoi, P., Pedersen, A. B., Gale, C. P., Smith, J. A., Maggioni, A. P., James, S., Fraser, A. G., Nelissen, R. G. H. H., & Marang-van de Mheen, P. J. (2023). Quality and Utility of European Cardiovascular and Orthopaedic Registries for the Regulatory Evaluation of Medical Device Safety and Performance Across the Implant Lifecycle: A Systematic Review. International journal of health policy and management, 12, 7648. https://doi.org/10.34172/ijhpm.2023.7648
- International Organization for Standardization. (2016). Medical devices — Quality management systems — Requirements for regulatory purposes (ISO Standard No. 13485:2016) https://www.iso.org/standard/59752.html
- International Organization for Standardization. (2019). Medical devices — Application of risk management to medical devices (ISO Standard No. 14971:2019) https://www.iso.org/standard/72704.html
- International Organization for Standardization. (2020). Clinical investigation of medical devices for human subjects — Good clinical practice (ISO Standard No. 14155:2020) https://www.iso.org/standard/71690.html
- Lee, H., Qureshi, A. M., Mueller-Kronast, N. H., Zaidat, O. O., Froehler, M. T., Liebeskind, D. S., & Pereira, V. M. (2021). Subarachnoid Hemorrhage in Mechanical Thrombectomy for Acute Ischemic Stroke: Analysis of the STRATIS Registry, Systematic Review, and Meta-Analysis. Frontiers in Neurology, 12, 663058. https://doi.org/10.3389/fneur.2021.663058
- Malenka, D. J., Bhatt, D. L., Bradley, S. M., Shahian, D. M., Draoui, J., Segawa, C. A., Koutras, C., Abbott, J. D., Blankenship, J. C., Vincent, R., Windle, J., Tsai, T. T., Curtis, J., Roe, M., & Masoudi, F. A. (2022). The National Cardiovascular Data Registry Data Quality Program 2020: JACC State-of-the-Art Review. Journal of the American College of Cardiology, 79(17), 1704–1712. https://doi.org/10.1016/j.jacc.2022.02.034
- Medical Device Coordination Group. (2019). Summary of safety and clinical performance (MDCG 2019-9) https://health.ec.europa.eu/medical-devices-sector/new-regulations/guidance-mdcg-endorsed-documents-and-other-guidance_en
- Medical Device Coordination Group. (2020). Guidance on PMCF evaluation report template (MDCG 2020-8) https://health.ec.europa.eu/medical-devices-sector/new-regulations/guidance-mdcg-endorsed-documents-and-other-guidance_en
- Medical Device Coordination Group. (2020). Guidance on PMCF plan template (MDCG 2020-7) https://health.ec.europa.eu/medical-devices-sector/new-regulations/guidance-mdcg-endorsed-documents-and-other-guidance_en
- Medical Device Coordination Group. (2020). Guidance on sufficient clinical evidence for legacy devices (MDCG 2020-6) https://health.ec.europa.eu/medical-devices-sector/new-regulations/guidance-mdcg-endorsed-documents-and-other-guidance_en
- Medical Device Coordination Group. (2022). Guidance on Periodic Safety Update Report (PSUR) according to Regulation (EU) 2017/745 (MDCG 2022-21) https://health.ec.europa.eu/medical-devices-sector/new-regulations/guidance-mdcg-endorsed-documents-and-other-guidance_en
- Medical Device Coordination Group. (2025). Guidance on post-market surveillance of medical devices and in vitro diagnostic medical devices (MDCG 2025-10) https://health.ec.europa.eu/medical-devices-sector/new-regulations/guidance-mdcg-endorsed-documents-and-other-guidance_en
- MedTech Europe. (2017). Medical Technology Registries – Six Key Principles https://www.medtecheurope.org/wp-content/uploads/2017/07/Medical-Technology-Registries-Six-Key-Principles-170509.pdf
- Naemi, R., Barikani, H. R., & Shahmoradi, L. (2021). Dental implant quality registries and databases: A systematic review. Journal of education and health promotion, 10, 214. https://doi.org/10.4103/jehp.jehp_1302_20
- Pascucci, S., Langella, F., Franzò, M., Tesse, M. G., Ciminello, E., Biondi, A., Carrani, E., Sampaolo, L., Zanoli, G., Berjano, P., & Torre, M. (2023). National spine surgery registries’ characteristics and aims: globally accepted standards have yet to be met. Results of a scoping review and a complementary survey. Journal of orthopaedics and traumatology : official journal of the Italian Society of Orthopaedics and Traumatology, 24(1), 49. https://doi.org/10.1186/s10195-023-00732-4
- Quigley, M., Apos, E., Truong, T. A., Ahern, S., & Johnson, M. A. (2023). Comorbidity data collection across different spine registries: an evidence map. European spine journal : official publication of the European Spine Society, the European Spinal Deformity Society, and the European Section of the Cervical Spine Research Society, 32(3), 753–777. https://doi.org/10.1007/s00586-023-07529-3
- Rubinger, L., Ekhtiari, S., Gazendam, A., & Bhandari, M. (2023). Registries: Big data, bigger problems? Injury, 54, S39-S42. https://doi.org/10.1016/j.injury.2021.12.016
- Sedrakyan, A., Marinac-Dabic, D., Campbell, B., Aryal, S., Baird, C. E., Goodney, P., Cronenwett, J. L., Beck, A. W., Paxton, E. W., Hu, J., Brindis, R., Baskin, K., Cowley, T., Levy, J., Liebeskind, D. S., Poulose, B. K., Rardin, C. R., Resnic, F. S., Tcheng, J., Fisher, B., … Pappas, G. (2022). Advancing the Real-World Evidence for Medical Devices through Coordinated Registry Networks. BMJ surgery, interventions, & health technologies, 4(Suppl 1), e000123. https://doi.org/10.1136/bmjsit-2021-000123
Disclaimer. The views and opinions expressed in this article are solely those of the author and do not necessarily reflect the official policy or position of Test Labs Limited. The content provided is for informational purposes only and is not intended to constitute legal or professional advice. Test Labs assumes no responsibility for any errors or omissions in the content of this article, nor for any actions taken in reliance thereon.
Get It Done, With Certainty.
Contact us about your testing requirements, we aim to respond the same day.
Get resources & industry updates direct to your inbox
We’ll email you 1-2 times a week at the maximum and never share your information


