
COP27
Last year the UK hosted COP26, the latest in a series of UN summits on climate change designed to help participating governments agree on steps to limit human impact on our climate system and global rises in temperature.
With COP27 now just days away, all eyes – including those of the National Health Service – will be on the goals and actions set at the summit and how their governments will respond to them.
Despite ongoing internal political and economic challenges, it still looks likely that the Government will remain committed to the long-term plan of its Net Zero Strategy: Build Back Greener that has set a goal of net zero by 2050.

A Net Zero National Health Service
NHS England is one of the largest contributors to greenhouse gas emissions in the UK, responsible for around 4% of the nation’s carbon emissions. This is hardly surprising as, with over 1.3 million employees, it is the largest employer in Britain and Europe. In fact, NHS England produces more CO2 per year than all passenger planes taking off from Heathrow annually.
This makes the NHS a prime target for Government CO2 reduction goals. Realising this, in 2020 the NHS launched its ‘For a greener NHS’ campaign and commissioned an Expert Panel to develop a roadmap towards becoming the world’s first net zero public health service.
Medical equipment currently accounts for 10% of the National Health Service’s total carbon footprint, so as further pressure is placed on the healthcare sector and its suppliers to deliver tangible results, medical device manufacturers need to understand how changes to NHS procurement policies will affect the future of MedTech.
How the NHS will achieve Net Zero
On 1 July 2022, the NHS became the first health system to embed net zero into legislation, through the Health and Care Act 2022 and with the ‘Delivering a Net Zero National Health Service report’ now issued as statutory guidance. This report sets out two clear and feasible targets:
- To reach net zero by 2040 for emissions the NHS controls directly
- To reach net zero by 2045 for emissions the NHS has the ability to influence.
These targets are ambitious and include assumptions about future innovations and the pace at which government, other sectors and the international community will drive change. They are also based on the scale of the challenge posed by climate change, as without adequate targets to reduce greenhouse gas emissions,
- disease patterns will change
- the frequency of extreme weather events will increase and
- demand for clinical services will rise across all social groups, both locally and globally.
Back in September 2021, the NHS England Public Board approved a roadmap to help suppliers align with NHS net zero ambition between now and 2030. This sets the following requirements:
- From April 2022 – all NHS procurements will include a minimum 10% net zero and social value weighting.
- From April 2023 – for all contracts above £5 million, the NHS will require suppliers to publish a carbon reduction plan for their UK Scope 1 and 2 emissions as a minimum
- From April 2024 – the NHS will extend the requirement for a carbon reduction plan to cover all procurements. Suppliers will be required to publish a carbon reduction plan for their UK Scope 1 and 2 as a minimum.
- From April 2027 – all suppliers will be required to publicly report targets, emissions and publish a carbon reduction plan for global emissions aligned to the NHS net zero target, for all of their Scope 1, 2 and 3 emissions.
- From April 2028 – new requirements will be introduced overseeing the provision of carbon foot printing for individual products supplied to the NHS. The NHS will work with suppliers and regulators to determine the scope and methodology.
- From 2030: suppliers will only be able to qualify for NHS contracts if they can demonstrate their progress through published progress reports and continued carbon emissions reporting through the Evergreen sustainable supplier assessment.
The NHS will continue to work closely with regulators, suppliers and industry bodies to shape their approach and give all suppliers the opportunity to align with their net zero ambition.

Net Zero NHS: the medical device reality
There are approximately 33,000 medical device manufacturers in Europe with a current value of €140 billion. The UK is the third largest market in Europe (12.1 %) with the NHS being the biggest consumer.
Since 2008, the NHS has tracked and reported its carbon footprint, regularly improving its methods and monitoring its progress in meeting the commitments of the Climate Change Act (2008). This Act set national targets for the reduction of carbon emissions in England against a 1990 baseline.
These targets do not, however, cover the full scope of emissions from the NHS. The Greenhouse Gas Protocol (GHGP) scopes cover a wider set of emissions and support international comparison and transparency:
- GHGP scope 1: Direct emissions from owned or directly controlled sources, on site
- GHGP scope 2: Indirect emissions from the generation of purchased energy, mostly electricity
- GHGP scope 3: All other indirect emissions that occur in producing and transporting goods and services, including the full supply chain.
Every area of the NHS will need to act if net zero is to be achieved, with the supply chain, estates and facilities, travel, and pharmaceuticals and medical devices being considered as the greatest areas of opportunity.
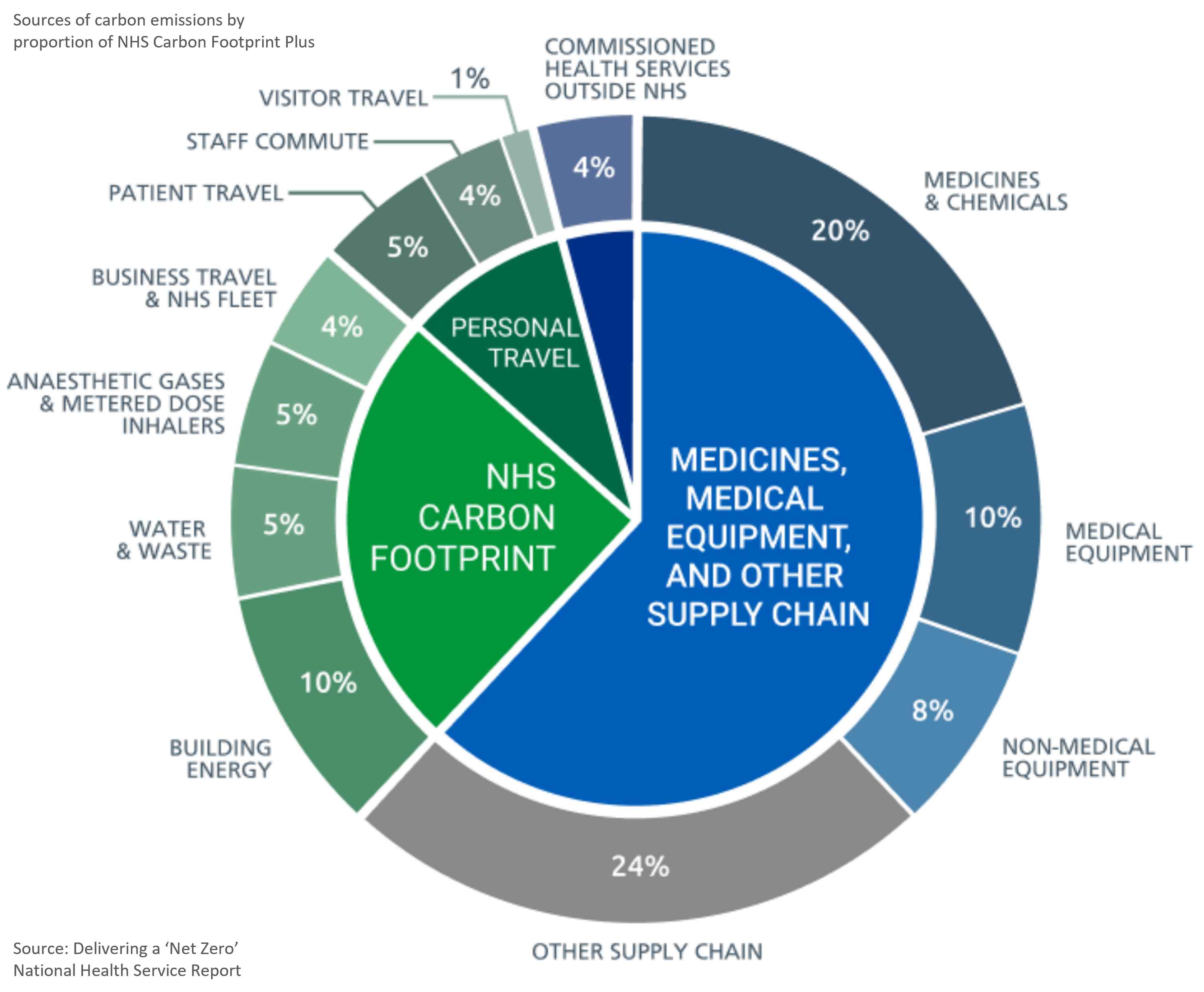
How can MedTech Manufacturers reach Net Zero?
As we have already mentioned, medical equipment accounts for 10% of total NHS carbon footprint – equivalent to the carbon footprint of all NHS patient, staff and visitor travel combined and double that of NHS water & waste.
Medical device manufacturers therefore play a key role in determining NHS success in reaching the targets it has set for the next three decades and one thing is certain – the NHS will be using its considerable purchasing power to drive required reductions in emissions. It is likely they will pursue this in three ways:
- More efficient use of supplies
- Low-carbon substitutions and product innovation
- Decarbonisation of suppliers’ own processes.
Medical device manufacturers must therefore develop their own Net Zero Strategy if they are to be able to continue supplying the NHS, Europe’s third-largest MedTech market.
How can this be done? Strategies that are being widely adopted by companies to achieve net zero include
- using green energy (switching to a green energy supplier, installing on-site photovoltaic (PV) panel or wind turbine power generation)
- converting to more energy-efficient manufacturing processes
- changing to a lower-carbon or carbon-neutral supply chain
- adopting smarter company travel policies (EV company vehicles, remote or hybrid working).
Net Zero Product Design and Manufacturing
At Test Labs, we see a further option open to medical device manufacturers: design and manufacture medical devices that offer longevity, reliability and compatibility with healthcare processes and you will immediately reduce the post-manufacture carbon footprint of your products.
Longevity – Medical devices that meet or exceed their expected lifespan both in terms of build quality and ‘future-proofness’ reduce carbon emissions created by premature replacements and upgrades.
Reusable alternatives to currently disposable products can also extend product life cycle and reduce carbon footprint.
Reliability – Medical devices that deliver fault-free service prevent the emissions generated by engineer callouts, emergency backup supplies, etc.
Compatibility – Medical devices should be compatible with all processes within the NHS for storage, use, infection prevention and control (wipes, consumables and technology) and end-of-life disposal (recycling, incineration, etc.).
The costs of replacing prematurely failing or breaking medical devices due to poor durability, unreliability and materials incompatibility all increase CO2 emissions unnecessarily, and place a financial burden on the healthcare provider: a co-published case study from the Healthcare Surfaces Institute revealed that just one medical device found to be incompatible with disinfection processes cost one hospital upwards of $4.1 million.
The NHS will look to reduce this residual through research and innovation. Net zero will be included in the NHS’ research strategy, and will inform engagement with industry, research centres of excellence and other key partners.
To ensure products meet these requirements, MedTech manufacturers must collaborate closely with the healthcare sector at all appropriate levels to understand and assess the full life cycle of their product, including how it is stored, used, cleaned and disposed of. They need feedback on its weaknesses and suggestions of how it can be improved.
The information gleaned from this collaboration, combined with design innovation and rigorous laboratory testing, will create a sound platform for developing medical devices that will help their manufacturers and the NHS meet net zero goals.

What happens next?
As the largest publicly funded health system in the world, the NHS annually
- admits 17 million inpatients from more than 200 hospital trusts
- handles more than 270 million primary care appointments from nearly 7,000 general practices
- prescribes more than 1.1 billion items.
This already high demand for healthcare services will continue to grow. However, the long-term target is clear: before the end of the decade, the NHS will no longer purchase from suppliers that do not meet or exceed their commitment to net zero.
Despite the political and economic pressures it is currently facing, the UK Government is unlikely to make a U-turn on its net zero commitments.
MedTech companies should therefore closely watch what statements the Government makes at COP27 and how it responds to the actions and agreements set out at the summit, particularly relating to NHS procurement strategies and policies.


